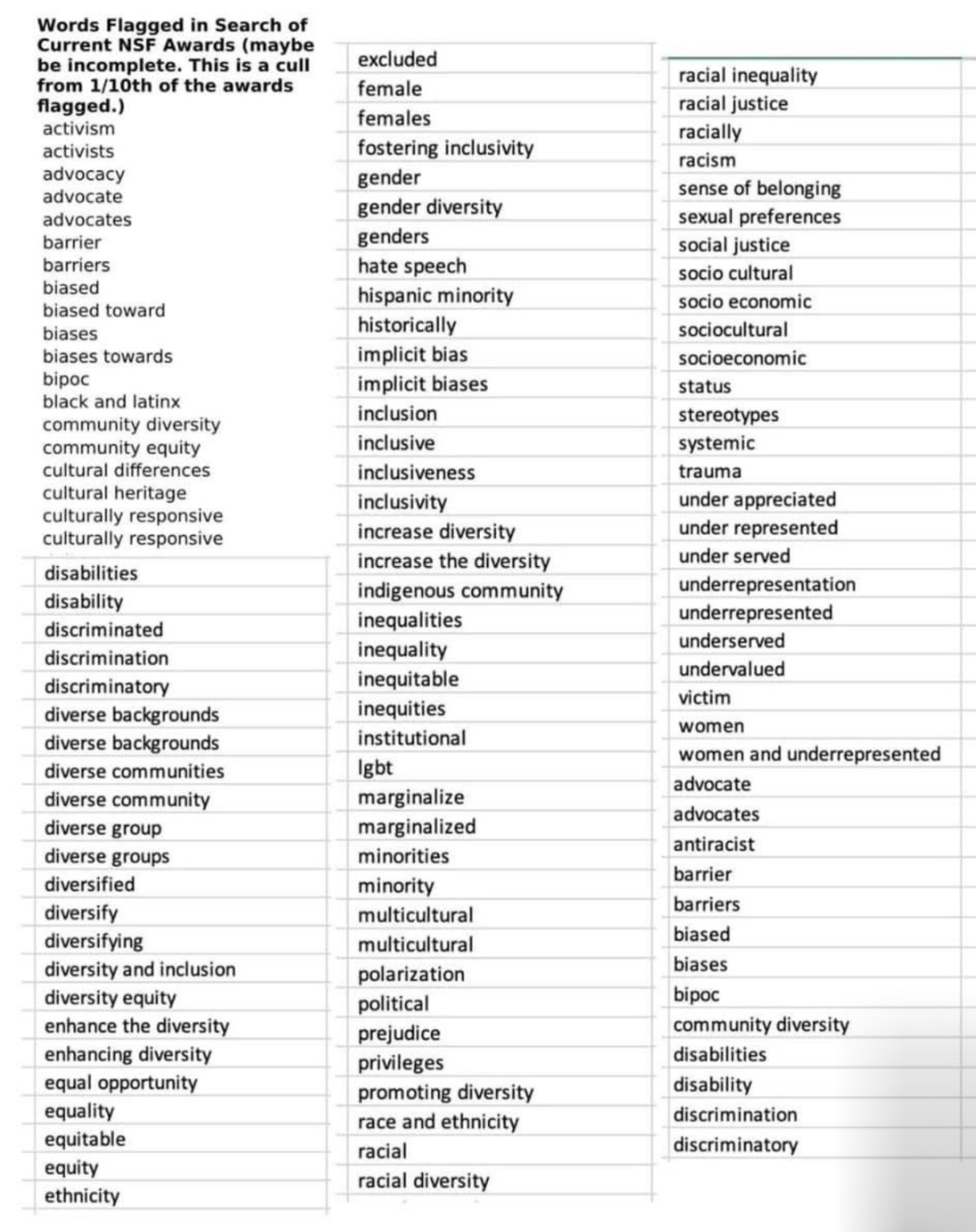
Much has been written lately about reframing word use in response to the latest generation of Executive Orders (EO) and other actions by the Federal Government. Yet, what happens when most of the words at issue are aligned with population health funding priorities as in accessibility, health equity, inclusion, or vulnerable populations? What happens when the words are commonly used in daily language, like advocate, expression, gender, or status? What happens when the words inform competencies for public health professions, as in cultural competence, implicit bias(es), oppression, or social justice? What happens when the words speak to evidence-based interventions that support populations across healthcare settings, such as anti-racism, cultural responsiveness, feminist, social justice, and trauma-informed? What happens when the words align with ethical codes of conduct and standards of practice for healthcare professionals whether discrimination, person-centered care, underserved, and vulnerable? What happens when shifting the words eliminates populations, persons, and their identities as in gender affirming, LGBTQIA, pronouns, Trans, or other terms. What happens when the list is ever-expanding and unpredictable? It is an understatement to say resolution is complicated.
How many ways are there to say, equitable, accessible, and quality-driven whole person healthcare? It presents there are many ways. Of course, the mantra remains that the more things we call these drivers and influencers of poor health outcomes and the persons who experience these factors the most, the less people will know what they are. These words have specific meanings; using so many different terms can invoke unintended misunderstandings. While the explicit intent of this new macro-focus is “to help Americans lead healthier lives” there is a clear and present worry that all populations may not be included in this mix.
Managing The Latest Information Flow
The constant attack on words is exhausting and frustrating to already weary professionals, practitioners, and providers, but most definitely patients and populations. This is an equally troublesome effort to those in higher education preparing future generations of the workforce.
The latest funding and programming shifts have left many reeling, including the March 2025 announcement to cease funding on four critical value-based care models: Primary Care First, End Stage Renal Disease Treatment Choices, the Maryland Total Cost of Care, and highly-anticipated Making Care Primary model. These shifts will impact millions of Medicaid and Chips recipients, plus Medicare beneficiaries with complex, costly chronic illnesses and the primary care practices that care for them.
This week saw Joint Commission reframe their highly coveted Health Equity Resource Center to reflect new verbiage of, The Optimal Delivery of Care for All; yes, the familiar language of “page not found” now appears when you one goes to the original website. History of Joint Commission’s focus in the health equity space is provided with emphasis on the entity’s ability to provide individual consultations to meet the new industry framing. In addition. CMS’s Health Equity Framework has been reframed as CMS’s Framework for Healthy Communities. The five pillars have also been reframed. In edition, their Health Equity Index used for Medicare Advantage Star Ratings has been rebranded as…..wait for it….The Excellent Health Outcomes for All Reward ((EHO4all). There is concern that the coveted 1115 Waivers might be next on the chopping block; time will tell.
Valuable time is being spent daily by colleagues to review, consider, and revamp programming to stop the ongoing rise of National Health Expenditures, expected to hit $5.3 Trillion. Much of my current bandwidth is spent staying current on policy and EO interpretations, but also supporting colleagues through job losses, or their fear of potential job losses. My students are coping with a constant flurry of issues from disappearing funding for their education and work-study programs to general concerns for their chosen career trajectory.
Here’s the Real Deal
Changing the terminology will not eliminate the wrath of health disparities and inequities experienced by historically minoritized and marginalized populations. Shifting words alone will do little to improve the poor clinical outcomes experienced by some populations more than others. Adjusting how populations are addressed will not decrease healthcare utilization or improve fiscal outcomes. Eliminating some populations from the conversation or funding will not dismiss the persons from those communities who experience worse illness morbidity and increased mortality rates. Reframing new initiatives will not identify the drivers of systemic racism, political determinants of health, and other social influencers of poor health for populations. In fact, each of these actions will further deteriorate the outputs of our current healthcare system. The US will continue its downward spiral of having the highest healthcare utilization and costs, along with the worse outcomes compared to other developed nations.
While we reconcile our fury about having to change longstanding terminology, the work to address the true priority at hand must continue. We must work to implement actionable strategies that heed our ethical obligations as healthcare professionals and providers. We must continue to advocate for ALL patients and their families so they receive access to the highest quality care available. That care must also be delivered to all in a fair and equitable way.
Strategies to Advance the Health Equity Equation
Emphasis needs to focus on defining, measuring, and incentivizing progress to improve access to quality care. A recent article in Health Affairs Scholar, posed clear direction with examples for each element provided. I encourage all to take a deeper dive into the piece to integrated these steps within your organization or practice:
- Define clear measures of equitable access and tracking progress at both organizational and national levels.
- Develop and implement equity-focused quality measures and aligned incentives to support progress and create accountability for addressing barriers in access to care (e.g., quality metrics, outcomes data).
- Health care leaders should undertake efforts to measure the availability and quality of health care services for people who experience inequitable access to health care and track progress towards addressing barriers to access (e.g. dashboard).
- Build and leverage cross-sector partnerships that allow collaboration on investing to address shared patient and community needs.
My daily dialogues with valued colleagues are a reminder to continue prioritizing ourselves and our energy. This will fuel our focus on the critical work at hand. Here are a few of my own strategies to push through this muck!
- Stay informed through your valued sources of intel but limit the amount of time spent viewing the information each day. While old habits have me check CMS Newsroom Posts weekly, there are other personal favorites: The Commonwealth Fund, Peterson/KFF System Tracker, Epstein Becker Green, and others.
- Explore what actionable strategies are up your sleeve
- Don’t silo your efforts: continue to discuss and strategize with colleagues who share your passion. Those relationships and conversations will continue to nurture and motivate your efforts.
- Try not to get lost in the alphabet soup of verbiage! Yes, it is toxic and traumatizing and will get the best of us if we let it! Instead, focus on actions to advance past the toxic energy around us. This may mean using alternative words or language, as posed in the list provided in the Federal Grant Trigger Words Replacement Workbook (yes, many alternatives were provided by ChatGPT).
- Stay up to date; the 4/3/25 document published by the EEOC and DOJ, What You Should Know About the Recent DEI-Related Discrimination at Work is a must read.
In the end, it is our actions that matter most to achieving the industry’s quality north star of the Quintuple Aim: patient- and family-centric care delivered at the right time, for the right cost, delivered by those who embrace the work, and assuring equitable access for all. Shifting words should not negate professional commitments and obligations to our patients, their families, and the workforce.